User:Mr. Ibrahem/Preterm birth
| Preterm birth | |
|---|---|
| Other names | Premature birth, preemies, premmies |
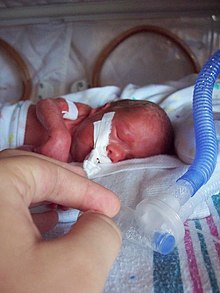 | |
| Intubated preterm baby in an incubator | |
| Specialty | Obstetrics, pediatrics |
| Symptoms | Birth of a baby at younger than 37 weeks' gestational age[1] |
| Complications | Cerebral palsy, delays in development, hearing problems, sight problems[1] |
| Causes | Often unknown[2] |
| Risk factors | Diabetes, high blood pressure, being pregnant with more than one baby, obesity or underweight, a number of vaginal infections, celiac disease, tobacco smoking, psychological stress[2][3][4] |
| Prevention | Progesterone[5] |
| Treatment | Corticosteroids, keeping the baby warm through skin-to-skin contact, supporting breastfeeding, treating infections, supporting breathing[2][6] |
| Frequency | ~15 million a year (12% of deliveries)[2] |
| Deaths | 805,800[7] |
Preterm birth, also known as premature birth, is the birth of a baby at fewer than 37 weeks' gestational age, as opposed to the usual about 40 weeks.[1] These babies are known as preemies or premmies.[1] Symptoms of preterm labor include uterine contractions which occur more often than every ten minutes or the leaking of fluid from the vagina.[8] Premature infants are at greater risk for cerebral palsy, delays in development, hearing problems and sight problems.[1] The earlier a baby is born, the greater these risks will be.[1]
The cause of preterm birth is often not known.[2] Risk factors include diabetes, high blood pressure, being pregnant with more than one baby, being either obese or underweight, a number of vaginal infections, air pollution including tobacco smoking, and psychological stress.[2][3][9] It is recommended that labor not be medically induced before 39 weeks unless required for other medical reasons.[2] The same recommendation applies to cesarean section.[2] Medical reasons for early delivery include preeclampsia.[10]
In those at risk, the hormone progesterone, if taken during pregnancy, may prevent preterm birth.[5] Evidence does not support the usefulness of bed rest.[5][11] It is estimated that at least 75% of preterm infants would survive with appropriate treatment, and the survival rate is highest among the infants born the latest.[2] In women who might deliver between 24 and 37 weeks, corticosteroids improve outcomes.[6][12] A number of medications, including nifedipine, may delay delivery so that a mother can be moved to where more medical care is available and the corticosteroids have a greater chance to work.[13] Once the baby is born, care includes keeping the baby warm through skin-to-skin contact, supporting breastfeeding, treating infections and supporting breathing.[2]
Preterm birth is the most common cause of death among infants worldwide.[1] About 15 million babies are preterm each year (5% to 18% of all deliveries).[2] In the United Kingdom they are about 7.9% and in the United States they are about 12.3% of all births.[14][15] Approximately 0.5% of births are extremely early periviable births, and these account for most of the deaths.[16] In many countries, rates of premature births have increased between the 1990s and 2010s.[2] Complications from preterm births resulted in 0.81 million deaths in 2015 down from 1.57 million in 1990.[7][17] The chance of survival at 22 weeks is about 6%, while at 23 weeks it is 26%, 24 weeks 55% and 25 weeks about 72%.[18] The chances of survival without any long-term difficulties are lower.[19]
References[edit]
- ^ a b c d e f g "Preterm Labor and Birth: Condition Information". National Institutes of Health. 3 November 2014. Archived from the original on 2 April 2015. Retrieved 7 March 2015.
- ^ a b c d e f g h i j k l World Health Organization (November 2014). "Preterm birth Fact sheet N°363". who.int. Archived from the original on 7 March 2015. Retrieved 6 March 2015.
- ^ a b "What are the risk factors for preterm labor and birth?". National Institutes of Health. 3 November 2014. Archived from the original on 5 April 2015. Retrieved 7 March 2015.
- ^ Saccone G, Berghella V, Sarno L, Maruotti GM, Cetin I, Greco L, Khashan AS, McCarthy F, Martinelli D, Fortunato F, Martinelli P (February 2016). "Celiac disease and obstetric complications: a systematic review and metaanalysis". American Journal of Obstetrics and Gynecology. 214 (2): 225–234. doi:10.1016/j.ajog.2015.09.080. PMID 26432464.
- ^ a b c "What treatments are used to prevent preterm labor and birth?". National Institutes of Health. 3 November 2014. Archived from the original on 2 April 2015. Retrieved 7 March 2015.
- ^ a b "What treatments can reduce the chances of preterm labor & birth?". National Institutes of Health. 11 June 2013. Archived from the original on 2 April 2015. Retrieved 7 March 2015.
- ^ a b Wang H, Naghavi M, Allen C, Barber RM, Bhutta ZA, Carter A, et al. (GBD 2015 Mortality and Causes of Death Collaborators) (October 2016). "Global, regional, and national life expectancy, all-cause mortality, and cause-specific mortality for 249 causes of death, 1980-2015: a systematic analysis for the Global Burden of Disease Study 2015". Lancet. 388 (10053): 1459–1544. doi:10.1016/s0140-6736(16)31012-1. PMC 5388903. PMID 27733281.
- ^ "What are the symptoms of preterm labor?". National Institutes of Health. 11 June 2013. Archived from the original on 2 April 2015. Retrieved 7 March 2015.
- ^ Korten, I; Ramsey, K; Latzin, P (January 2017). "Air pollution during pregnancy and lung development in the child". Paediatric Respiratory Reviews. 21: 38–46. doi:10.1016/j.prrv.2016.08.008. PMID 27665510.
- ^ "What causes preterm labor and birth?". National Institutes of Health. 3 November 2014. Archived from the original on 2 April 2015. Retrieved 7 March 2015.
- ^ Sosa CG, Althabe F, Belizán JM, Bergel E (March 2015). "Bed rest in singleton pregnancies for preventing preterm birth". The Cochrane Database of Systematic Reviews. 3 (3): CD003581. doi:10.1002/14651858.CD003581.pub3. PMC 7144825. PMID 25821121.
- ^ "Antenatal Corticosteroid Therapy for Fetal Maturation". ACOG. October 2016. Archived from the original on 29 September 2016. Retrieved 27 September 2016.
- ^ Haram K, Mortensen JH, Morrison JC (March 2015). "Tocolysis for acute preterm labor: does anything work". The Journal of Maternal-Fetal & Neonatal Medicine. 28 (4): 371–8. doi:10.3109/14767058.2014.918095. PMID 24990666. S2CID 20078137.
- ^ Chow, Yuan Huang; Dattani, Nirupa (2009-02-26). "Estimating conception statistics using gestational age information from NHS Numbers for Babies data". Health Statistics Quarterly. 41 (1): 21–27. doi:10.1057/hsq.2009.5. ISSN 2040-1574. PMID 19320250. S2CID 23996035.
- ^ Mathews, T. J.; Minino, A. M.; Osterman, M. J. K.; Strobino, D. M.; Guyer, B. (2010-12-20). "Annual Summary of Vital Statistics: 2008". Pediatrics. 127 (1): 146–157. doi:10.1542/peds.2010-3175. ISSN 0031-4005. PMC 4079290. PMID 21173001.
- ^ American College of Obstetricians Gynecologists; Society for Maternal-Fetal Medicine (October 2017). "Obstetric Care consensus No. 6: Periviable Birth". Obstetrics and Gynecology. 130 (4): e187–e199. doi:10.1097/AOG.0000000000002352. PMID 28937572.
- ^ GBD 2013 Mortality and Causes of Death Collaborators (January 2015). "Global, regional, and national age-sex specific all-cause and cause-specific mortality for 240 causes of death, 1990-2013: a systematic analysis for the Global Burden of Disease Study 2013". Lancet. 385 (9963): 117–71. doi:10.1016/S0140-6736(14)61682-2. PMC 4340604. PMID 25530442.
{{cite journal}}:|author=has generic name (help)CS1 maint: numeric names: authors list (link) - ^ Cloherty and Stark's Manual of Neonatal Care (8 ed.). Lippincott Williams & Wilkins. 2016. p. 161. ISBN 9781496367495.
- ^ Jarjour IT (February 2015). "Neurodevelopmental outcome after extreme prematurity: a review of the literature". Pediatric Neurology. 52 (2): 143–52. doi:10.1016/j.pediatrneurol.2014.10.027. PMID 25497122.
