Abdominal aortic aneurysm: Difference between revisions
Changed third intro paragraph to include EVAR ~~~~~ |
|||
| Line 19: | Line 19: | ||
Abdominal aortic aneurysms occur most commonly in individuals between 65 and 75 years old and are more common among men and smokers. They tend to cause no symptoms, although occasionally they cause [[pain]] in the abdomen and back (due to pressure on surrounding tissues) or in the legs (due to disturbed blood flow). The major complication of abdominal aortic aneurysms is rupture, which is life-threatening, as large amounts of blood spill into the [[abdominal cavity]], and can lead to death within minutes.<ref name=AAFP>{{cite journal |author=Upchurch GR, Schaub TA |title=Abdominal aortic aneurysm |journal=Am Fam Physician |volume=73 |issue=7 |pages=1198–204 |year=2006 |pmid=16623206 }}</ref> Mortality of rupture repair in the hospital is 60% to 90%. |
Abdominal aortic aneurysms occur most commonly in individuals between 65 and 75 years old and are more common among men and smokers. They tend to cause no symptoms, although occasionally they cause [[pain]] in the abdomen and back (due to pressure on surrounding tissues) or in the legs (due to disturbed blood flow). The major complication of abdominal aortic aneurysms is rupture, which is life-threatening, as large amounts of blood spill into the [[abdominal cavity]], and can lead to death within minutes.<ref name=AAFP>{{cite journal |author=Upchurch GR, Schaub TA |title=Abdominal aortic aneurysm |journal=Am Fam Physician |volume=73 |issue=7 |pages=1198–204 |year=2006 |pmid=16623206 }}</ref> Mortality of rupture repair in the hospital is 60% to 90%. |
||
Treatment is usually recommended when an AAA grows to >5.5 cm in diameter. While in the past the only option for the treatment of AAA was open surgery, today most are treated with Endovascular Aneurysm Repair ([[EVAR]]).<ref name=JVS>{{cite journal |author=Chadi SA et al |title=Trends in management of abdominal aortic aneurysms |journal=J Vasc Surg|volume=55 |issue=4 |pages=924-8 |year=2012 |pmid= 22226189}}</ref> EVAR has been widely adopted, as EVAR has a lower risk of death associated with surgery (0.5 for EVAR vs 3 for open surgery).<ref name=JAMA>{{cite journal |author=Lederle FA, Freishlag JA et al |title=Outcomes Following Endovascular vs Open Repair of Abdominal Aortic Aneurysm: A Randomized Trial |journal=JAMA|volume=302 |issue=14 |pages=1535-42 |year=209 |pmid= 19826022}}</ref> Open surgery is sometimes still preferred to EVAR, as EVAR requires long-term surveillance with [[Computed tomography of the abdomen and pelvis|CT Scans]].<ref name=Ann Vasc Surg>{{cite journal |author=Kirkpatrick VE et al |title=Surveillance Computed Tomographic Arteriogram (CTA) Does Not Change Management before Three Years in Patients Who Have a Normal Post-EVAR Study|journal=Ann Vasc Surg| year: Epub ahead of print |pmid= 24361383}}</ref> |
|||
Surgery is recommended when the aneurysm is large enough (>5.5 cm in diameter). With newer procedures, surgical risk is minimal – much less than the risk of rupture. Open surgery is a viable option to stents, particularly when one chooses to avoid the issues associated with routine stent replacement or early failure. A stent consists of a stainless steel mesh liner inserted through the groin and put in place with endoscopic tools, then spread with a balloon-like device to hold the [[stent]] in place. Yearly CT scans are necessary to determine if the mesh tube stents have failed and require replacement. |
|||
There is moderate evidence to support [[screening (medicine)|screening]] in individuals with risk factors for abdominal aortic aneurysms (e.g., males ≥65). |
There is moderate evidence to support [[screening (medicine)|screening]] in individuals with risk factors for abdominal aortic aneurysms (e.g., males ≥65). |
||
Revision as of 20:28, 6 March 2014
| Abdominal aortic aneurysm | |
|---|---|
| Specialty | Vascular surgery |
Abdominal aortic aneurysm (also known as AAA, pronounced "triple-a") is a localized dilatation (ballooning) of the abdominal aorta exceeding the normal diameter by more than 50 percent, and is the most common form of aortic aneurysm. Approximately 90 percent of abdominal aortic aneurysms occur infrarenally (below the kidneys), but they can also occur pararenally (at the level of the kidneys) or suprarenally (above the kidneys). Such aneurysms can extend to include one or both of the iliac arteries in the pelvis.
Abdominal aortic aneurysms occur most commonly in individuals between 65 and 75 years old and are more common among men and smokers. They tend to cause no symptoms, although occasionally they cause pain in the abdomen and back (due to pressure on surrounding tissues) or in the legs (due to disturbed blood flow). The major complication of abdominal aortic aneurysms is rupture, which is life-threatening, as large amounts of blood spill into the abdominal cavity, and can lead to death within minutes.[1] Mortality of rupture repair in the hospital is 60% to 90%.
Treatment is usually recommended when an AAA grows to >5.5 cm in diameter. While in the past the only option for the treatment of AAA was open surgery, today most are treated with Endovascular Aneurysm Repair (EVAR).[2] EVAR has been widely adopted, as EVAR has a lower risk of death associated with surgery (0.5 for EVAR vs 3 for open surgery).[3] Open surgery is sometimes still preferred to EVAR, as EVAR requires long-term surveillance with CT Scans.Cite error: The <ref> tag has too many names (see the help page).
There is moderate evidence to support screening in individuals with risk factors for abdominal aortic aneurysms (e.g., males ≥65).
Classification
Abdominal aortic aneurysms are commonly divided according to their size and symptomatology. An aneurysm is usually defined as an outer aortic diameter over 3 cm (normal diameter of the aorta is around 2 cm).[4] If the outer diameter exceeds 5.5 cm, the aneurysm is considered to be large.[5] A ruptured AAA is a clinical diagnosis involving the presence of the triad of abdominal pain, shock and a pulsatile abdominal mass. If these conditions are present, indicating AAA rupture, no further clinical investigations are needed before surgery.[6]
Signs and symptoms

The vast majority of aneurysms are asymptomatic. However, as abdominal aortic aneurysms expand, they may become painful and lead to pulsating sensations in the abdomen or pain in the chest, lower back, or scrotum.[7] The risk of rupture is high in a symptomatic aneurysm, which is therefore considered an indication for surgery. The complications include rupture, peripheral embolization, acute aortic occlusion, and aortocaval (between the aorta and inferior vena cava) or aortoduodenal (between the aorta and the duodenum) fistulae. On physical examination, a palpable abdominal mass can be noted. Bruits can be present in case of renal or visceral arterial stenosis.[8]
The clinical manifestation of ruptured AAA usually includes excruciating pain of the lower back, flank, abdomen and groin. The bleeding usually leads to a hypovolemic shock with hypotension, tachycardia, cyanosis, and altered mental status. The mortality of AAA rupture is up to 90%. 65–75% of patients die before they arrive at hospital and up to 90% die before they reach the operating room.[9] The bleeding can be retroperitoneal or intraperitoneal, or the rupture can create an aortocaval or aortointestinal (between the aorta and intestine) fistula.[10] Flank ecchymosis (appearance of a bruise) is a sign of retroperitoneal hemorrhage, and is also called Grey Turner's sign.[8][11]
Causes
The exact causes of the degenerative process remain unclear. There are, however, some hypotheses and well-defined risk factors.[12]
- Tobacco smoking: Greater than 90% of people who develop an AAA have smoked at some point in their life.[13]
- Alcohol and hypertension: The inflammation caused by prolonged use of alcohol and hypertensive effects from abdominal edema which leads to hemorrhoids, esophageal varices, and other conditions, is also considered a long-term cause of AAA.
- Genetic influences: The influence of genetic factors is highly probable. The high familial prevalence rate is most notable in male individuals.[14] There are many hypotheses about the exact genetic disorder that could cause higher incidence of AAA among male members of the affected families. Some presumed that the influence of alpha 1-antitrypsin deficiency could be crucial, while other experimental works favored the hypothesis of X-linked mutation, which would explain the lower incidence in heterozygous females. Other hypotheses of genetic etiology have also been formulated.[8] Connective tissue disorders, such as Marfan syndrome and Ehlers-Danlos syndrome, have also been strongly associated with AAA.[10] Both relapsing polychondritis and pseudoxanthoma elasticum may cause abdominal aortic aneurysm.[15]
- Atherosclerosis: The AAA was long considered to be caused by atherosclerosis, because the walls of the AAA are frequently affected heavily. However, this hypothesis cannot be used to explain the initial defect and the development of occlusion, which is observed in the process.[8]
- Other causes: Other causes of the development of AAA include: infection, trauma, arteritis, cystic medial necrosis (m. Erdheim).[10]
Pathophysiology
The most striking histopathological changes of aneurysmatic aorta are seen in tunica media and intima. These include accumulation of lipids in foam cells, extracellular free cholesterol crystals, calcifications, thrombosis, and ulcerations and ruptures of the layers. There is an adventitial inflammatory infiltrate.[10] However, the degradation of tunica media by means of proteolytic process seems to be the basic pathophysiologic mechanism of the AAA development. Some researchers report increased expression and activity of matrix metalloproteinases in individuals with AAA. This leads to elimination of elastin from the media, rendering the aortic wall more susceptible to the influence of the blood pressure.[8] There is also a reduced amount of vasa vasorum in the abdominal aorta (compared to the thoracic aorta); consequently, the tunica media must rely mostly on diffusion for nutrition which makes it more susceptible to damage.[16]
Hemodynamics affect the development of AAA. It has a predilection for the infrarenal aorta. The histological structure and mechanical characteristics of infrarenal aorta differ from those of the thoracic aorta. The diameter decreases from the root to the bifurcation, and the wall of the abdominal aorta also contains a lesser proportion of elastin. The mechanical tension in abdominal aortic wall is therefore higher than in the thoracic aortic wall. The elasticity and distensibility also decline with age, which can result in gradual dilatation of the segment. Higher intraluminal pressure in patients with arterial hypertension markedly contributes to the progression of the pathological process.[10] Suitable hemodynamics conditions may be linked to specific Intraluminal Thrombus (ILT) patterns along the aortic lumen, which in turn may affect AAA's development.[17]
Diagnosis
An abdominal aortic aneurysm is usually diagnosed by physical exam, ultrasound, or CT. Plain abdominal radiographs may show the outline of an aneurysm when its walls are calcified. However, this is the case in less than half of all aneurysms. Ultrasonography is used to screen for aneurysms and to determine the size of any present. Additionally, free peritoneal fluid can be detected. It is noninvasive and sensitive, but the presence of bowel gas or obesity may limit its usefulness. CT scan has a nearly 100% sensitivity for aneurysm and is also useful in preoperative planning, detailing the anatomy and possibility for endovascular repair. In the case of suspected rupture, it can also reliably detect retroperitoneal fluid. Alternative less often used methods for visualization of the aneurysm include MRI and angiography.
An aneurysm ruptures if the mechanical stress (tension per area) exceeds the local wall strength; consequently, peak wall stress (PWS) [18] and peak wall rupture risk (PWRR) [19] have been found to be more reliable parameters than diameter to assess AAA rupture risk. Medical software allows computing these rupture risk indices from standard clinical CT data and provides a patient-specific AAA rupture risk diagnosis.[20]
-
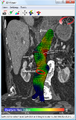
A ruptured AAA with an open arrow marking the aneurysm and the closed arrow marking the free blood in the abdomen
-
Sagittal CT image of an AAA.
-
Biomechanical AAA Rupture risk prediction.
-
An axial contrast enhanced CT scan demonstrating an abdominal aortic aneurysm of 4.8 by 3.8 cm
-
Ultrasound image of a normal abdominal aorta measuring 1.9 cm in diameter.
-
The faint outline of the calcified wall of a AAA as seen on plain X-ray
-
CT image of an AAA 40,8 mm.
-
Abdominal aortic aneurysms (3,4 cm)
Prevention
- Treatment of hypertension
- Smoking cessation
- Low-fat diet
- Screening abdominal ultrasound for men older than 65 years has been shown to reduce mortality, although cost-effectiveness has not been shown.
Screening
The U.S. Preventive Services Task Force recommends a single screening ultrasound for abdominal aortic aneurysm in males age 65 to 75 years who have a history of smoking.[21][22] There is an estimated number needed to screen of approximately 850 patients.[23] Screening is not recommended in women.[21]
Repeat ultrasounds should be carried out in those who have an aortic size greater than 3.0 cm.[24] In those whose aorta is between 3.0 and 3.9 cm this should be every three years, if between 4.0 and 4.4 cm every two year, and if between 4.5 and 5.4 cm every year.[24]
Management
The treatment options for asymptomatic AAA are conservative management, surveillance with a view to eventual repair, and immediate repair. There are currently two modes of repair available for an AAA: open aneurysm repair (OR), and endovascular aneurysm repair (EVAR). An intervention is often recommended if the aneurysm grows more than 1 cm per year or it is bigger than 5.5 cm.[13] Repair is also indicated for symptomatic aneurysms.[25]
Conservative
Conservative management is indicated in patients where repair carries a high risk of mortality and in patients where repair is unlikely to improve life expectancy. The mainstay of the conservative treatment is smoking cessation.
Surveillance is indicated in small asymptomatic aneurysms (less than 5.5 cm) where the risk of repair exceeds the risk of rupture. As an AAA grows in diameter the risk of rupture increases. Surveillance until the aneurysm has reached a diameter of 5.5 cm has not been shown to have a higher risk as compared to early intervention.[26][27]
Medication
No medical therapy has been found to be effective at decreasing the growth rate or rupture rate of asymptomatic AAAs.[25] Blood pressure and lipids should however be treated like in any atherosclerotic condition.[4] Studies have suggested possible protective effects of therapy with angiotensin converting enzyme inhibitors,[28] beta-blockers,[4] and statins.[29]
Surgery
Surgery for an abdominal aortic aneurysm is known as AAA surgery or AAA repair. The threshold for repair varies slightly from individual to individual, depending on the balance of risks and benefits when considering repair versus ongoing surveillance. The size of an individual's native aorta may influence this, along with the presence of comorbidities that increase operative risk or decrease life expectancy.[25]
- Open repair
Open repair is indicated in young patients as an elective procedure, or in growing or large, symptomatic or ruptured aneurysms. It was the main surgical intervention used from the 1950s until other procedures developed.
For most operations, the surgeon tries to use as small an incision as reasonably possible, but that is not the case for open AAA surgery because there is an overriding concern. The aorta must be clamped off during the repair, and that denies blood to the entire abdomen and both legs; this can cause a whole range of complications if the aorta is shut off too long. It is essential to make the critical part of the operation fast, so the incision is typically made as large as possible, from just below the breastbone to just above the pubic bone.
Recovery after open AAA surgery takes significant time. The minimums are a few days in intensive care, a week total time in hospital and a few months before full recovery.
- Endovascular repair

Endovascular repair first became practical in the 1990s and although it is now an established alternative to open repair, its role is yet to be clearly defined. It is generally indicated in older, high-risk patients or patients unfit for open repair. However, endovascular repair is feasible for only a proportion of AAAs, depending on the morphology of the aneurysm. The main advantages over open repair are that there is less peri-operative mortality, less time in intensive care, less time in hospital overall and earlier return to normal activity. Disadvantages of endovascular repair include a requirement for more frequent ongoing hospital reviews, and a higher chance of further procedures being required. According to the latest studies, the EVAR procedure does not offer any benefit for overall survival or health-related quality of life compared to open surgery, although aneurysm-related mortality is lower.[30][31][32][33] In patients unfit for open repair, EVAR plus conservative management was associated with no benefit, more complications, subsequent procedures and higher costs compared to conservative management alone.[34] Endovascular treatment for paraanastomotic aneurysms after aortobiiliac reconstruction is also a possibility.[35]
A major cause of complications in EVAR is the failure of the seal between the proximal, infra-renal aneurysm neck and the endovascular graft.[36][37][38] Risk of this form of failure is especially elevated in adverse or challenging proximal neck anatomies, where this seal could be compromised by unsuitable geometric fit between the graft and vessel wall, as well as instability of the anatomy.[39][40][41] New recent techniques have been introduced to address these risks by utilizing a segment of the supra-renal portion of the aorta to increase the sealing zone, such as with fenestrated EVAR, chimneys and snorkels.[42] These techniques may be suitable in certain patients with qualifying factors, e.g. configuration of renal arteries, renal function. However, these are more complex procedures than standard EVAR and may be subject to further complications.[43][44][45]
An approach that directly augments the fixation and sealing between the graft and aorta to mimic the stability of a surgical anastomosis is EndoAnchoring.[46][47] EndoAnchors are small, helically-shaped implants that directly lock the graft to the aortic wall with the goal to prevent complications of the seal, especially in adverse neck anatomies.[48][49] These EndoAnchors may also be used to treat identified leaks between the graft and proximal neck.[50][51][52] To ensure successful implantation, placement of EndoAnchors should be limited to the areas of the aortic neck free from excessive thrombus, calcification and/or plaque.
Prognosis
| AAA Size (cm) | Growth rate (cm/yr)[53] | Annual rupture risk (%)[54] |
|---|---|---|
| 3.0-3.9 | 0.39 | 0 |
| 4.0-4.9 | 0.36 | 0.5-5 |
| 5.0-5.9 | 0.43 | 3-15 |
| 6.0-6.9 | 0.64 | 10-20 |
| >=7.0 | - | 20-50 |
Although the current standard of determining rupture risk is based on maximum diameter, it is known that smaller AAAs that fall below this threshold (diameter<5.5 cm) may also rupture, and larger AAAs (diameter>5.5 cm) may remain stable.[55][56] In one report, it was shown that 10–24% of ruptured AAAs were less than 5 cm in diameter.[56] It has also been reported that of 473 non-repaired AAAs examined from autopsy reports, there were 118 cases of rupture, 13% of which were less than 5 cm in diameter. This study also showed that 60% of the AAAs greater than 5 cm (including 54% of those AAAs between 7.1 and 10 cm) never experienced rupture.[57] Vorp et al. later deduced from the findings of Darling et al. that if the maximum diameter criterion were followed for the 473 subjects, only 7% (34/473) of cases would have succumbed to rupture prior to surgical intervention as the diameter was less than 5 cm, with 25% (116/473) of cases possibly undergoing unnecessary surgery since these AAAs may never have ruptured.[57]
Alternative methods of rupture assessment have been recently reported. The majority of these approaches involve the numerical analysis of AAAs using the common engineering technique of the finite element method (FEM) to determine the wall stress distributions. Recent reports have shown that these stress distributions have been shown to correlate to the overall geometry of the AAA rather than solely to the maximum diameter.[58][59][60] It is also known that wall stress alone does not completely govern failure as an AAA will usually rupture when the wall stress exceeds the wall strength. In light of this, rupture assessment may be more accurate if both the patient-specific wall stress is coupled together with patient-specific wall strength. A non-invasive method of determining patient-dependent wall strength was recently reported,[61] with more traditional approaches to strength determination via tensile testing performed by other researchers in the field.[62][63][64] Some of the more recently proposed AAA rupture-risk assessment methods include: AAA wall stress;[18][65][66] AAA expansion rate;[67] degree of asymmetry;[60] presence of intraluminal thrombus (ILT);[68] a rupture potential index (RPI);[69][70] a finite element analysis rupture index (FEARI);[71] biomechanical factors coupled with computer analysis;[72] growth of ILT;[73] geometrical parameters of the AAA;[74] and also a method of determining AAA growth and rupture based on mathematical models.[75][76]
The post-operative mortality for an already ruptured AAA has slowly decreased over several decades but remains higher than 40%.[6] However, if the AAA is surgically repaired before rupture, the post-operative mortality rate is substantially lower: approximately 1-6%.[77]
Epidemiology
The occurrence of AAA varies markedly by ethnicity. In the United Kingdom the rate of AAA in Caucasian men older than 65 years is about 4.7%, while in Asian men it is 0.45%.[78] It is also uncommon in individuals of African, and Hispanic heritage.[citation needed]
There are 9000 deaths yearly in the U.S. secondary to AAA rupture.[79] The frequency varies strongly between males and females. The peak incidence is among males around 70 years of age, the prevalence among males over 60 years totals 2-6%. The frequency is much higher in smokers than in non-smokers (8:1), and the risk decreases slowly after smoking cessation.[80] Other risk factors include hypertension and male sex.[10] In the U.S., the incidence of AAA is 2-4% in the adult population.[8] AAA is 4-6 times more common in male siblings of known patients, with a risk of 20-30%.[81]
Rupture of the AAA occurs in 1-3% of men aged 65 or more, the mortality is 70-95%.[5]
History
The first historical records about AAA are from Ancient Rome in the 2nd century AD, when Greek surgeon Antyllus tried to treat the AAA with proximal and distal ligature, central incision and removal of thrombotic material from the aneurysm. However, attempts to treat the AAA surgically were unsuccessful until 1923. In that year, Rudolph Matas (who also proposed the concept of endoaneurysmorrhaphy), performed the first successful aortic ligation on a human.[82] Other methods that were successful in treating the AAA included wrapping the aorta with polyethene cellophane, which induced fibrosis and restricted the growth of the aneurysm. Albert Einstein was operated on by Rudolph Nissen with use of this technique in 1949, and survived five years after the operation, though he eventually died when the aneurysm ruptured.[83] Endovascular aneurysm repair was first performed in the late 1980s and has been widely adopted in the subsequent decades. Endovascular repair was first used for treating a ruptured aneurysm in Nottingham in 1994[84]
Former presidential candidate Bob Dole had an abdominal aortic aneurysm in 2001 and was treated surgically by vascular surgeon Kenneth Ouriel. The operation was successful. In 1993, country music singer Conway Twitty died from AAA.[85]
Society and culture
In 2001 former presidential candidate Bob Dole underwent surgery for an abdominal aortic aneurysm in which a team of surgeons led by Doctor Kenneth Ouriel inserted a stent graft:
Ouriel said that the team inserted a Y-shaped tube through an incision in Dole's leg and placed it inside the weakened portion of the aorta. The aneurysm will eventually contract around the stent, which will remain in place for the rest of Dole's life.[85]
Research
Risk assessment and experimental models
There have been many calls for alternative approaches to rupture-risk assessment over the past number of years, with many believing that a biomechanics-based approach may be more suitable than the current diameter approach. Numerical modelling is a valuable tool to researchers allowing approximate wall stresses to be calculated, thus revealing the rupture potential of a particular aneurysm. Experimental models are required to validate these numerical results, and provide a further insight into the biomechanical behaviour of the AAA. In vivo, AAAs exhibit a varying range of material strengths[86] from localised weak hypoxic regions[87] to much stronger regions and areas of calcifications.[88] Experimental models can now be manufactured using a novel technique involving the injection-moulding lost-wax manufacturing process to create patient-specific anatomically-correct AAA replicas.[89] Work has also focused on developing more realistic material analogues to those in vivo, and recently a novel range of silicone-rubbers was created allowing the varying material properties of the AAA to be more accurately represented.[90] These rubber models can also be used in a variety of experimental testing from stress analysis using the photoelastic method[91] to deterimining whether the locations of rupture experimentally correlate with those predicted numerically.[92] New endovascular devices are being developed that are able to treat more complex and tortuous anatomies.[93]
Prevention and treatment
A recent animal study published in the journal Nature Medicine showed that removing a single protein prevents early damage in blood vessels from triggering a later-stage, frequently lethal complication of atherosclerosis. By eliminating the gene for a signaling protein called cyclophilin A (CypA) from a strain of mice, researchers were able to provide complete protection against abdominal aortic aneurysm (AAA).[94]
Other recent research, published in the American Journal of Pathology, identified Granzyme B (GZMB) (a protein-degrading enzyme) to be a potential therapeutic target in the treatment of abdominal aortic aneurysms. Specifically, elimination of this enzyme in mice models — both slowed the progression of aneurysms and improved survival.[95][96]
With the recent advancements in AAA research, coupled with the increasing collaboration between clinicians and engineers, the future research into AAA rupture-prediction and treatment appears to be in a strong position to combat what is currently ranked as the 13th leading cause of death in the US and the 10th leading cause of death in men over the age of 55 years.
References
- ^ Upchurch GR, Schaub TA (2006). "Abdominal aortic aneurysm". Am Fam Physician. 73 (7): 1198–204. PMID 16623206.
- ^ Chadi SA; et al. (2012). "Trends in management of abdominal aortic aneurysms". J Vasc Surg. 55 (4): 924–8. PMID 22226189.
{{cite journal}}: Explicit use of et al. in:|author=(help) - ^ Lederle FA, Freishlag JA; et al. (209). "Outcomes Following Endovascular vs Open Repair of Abdominal Aortic Aneurysm: A Randomized Trial". JAMA. 302 (14): 1535–42. PMID 19826022.
{{cite journal}}: Explicit use of et al. in:|author=(help) - ^ a b c Hirsch AT, Haskal ZJ, Hertzer NR; et al. (September 2006). "ACC/AHA Guidelines for the Management of Patients with Peripheral Arterial Disease (lower extremity, renal, mesenteric, and abdominal aortic): a collaborative report from the American Associations for Vascular Surgery/Society for Vascular Surgery, Society for Cardiovascular Angiography and Interventions, Society for Vascular Medicine and Biology, Society of Interventional Radiology, and the ACC/AHA Task Force on Practice Guidelines (writing committee to develop guidelines for the management of patients with peripheral arterial disease)—summary of recommendations". J Vasc Interv Radiol. 17 (9): 1383–97, quiz 1398. doi:10.1097/01.RVI.0000240426.53079.46. PMID 16990459.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ a b Lindholt JS, Juul S, Fasting H, Henneberg EW (Apr 2005). "Screening for abdominal aortic aneurysms: single centre randomised controlled trial". BMJ. 330 (7494): 750. doi:10.1136/bmj.38369.620162.82. PMC 555873. PMID 15757960.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ a b Bown MJ, Sutton AJ, Bell PR, Sayers RD (June 2002). "A meta-analysis of 50 years of ruptured abdominal aortic aneurysm repair". The British Journal of Surgery. 89 (6): 714–30. doi:10.1046/j.1365-2168.2002.02122.x. PMID 12027981.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Fauci, Anthony (2008-03-06). "242". Harrison's Principles of Internal Medicine (17 ed.). McGraw-Hill Professional. ISBN 0-07-146633-9.
- ^ a b c d e f Abdominal Aortic Aneurysm at eMedicine
- ^ Brown LC, Powell JT (September 1999). "Risk Factors for Aneurysm Rupture in Patients Kept Under Ultrasound Surveillance". Annals of Surgery. 230 (3): 289–96, discussion 296–7. doi:10.1097/00000658-199909000-00002. PMC 1420874. PMID 10493476.
- ^ a b c d e f Treska V. et al.:Aneuryzma břišní aorty, Prague, 1999, ISBN 80-7169-724-9
- ^ Goldman, Lee. Goldman's Cecil Medicine (24th ed. ed.). Philadelphia: Elsevier Saunders. p. 837. ISBN 1437727883.
{{cite book}}:|edition=has extra text (help) - ^ http://www.danmedbul.dk/portal/pls/portal/docs/6348849.PDF
- ^ a b Greenhalgh RM, Powell JT (January 2008). "Endovascular repair of abdominal aortic aneurysm". N. Engl. J. Med. 358 (5): 494–501. doi:10.1056/NEJMct0707524. PMID 18234753.
- ^ Clifton MA (Nov 1977). "Familial abdominal aortic aneurysms". Br J Surg. 64 (11): 765–6. doi:10.1002/bjs.1800641102. PMID 588966.
- ^ Rapini, Ronald P.; Bolognia, Jean L.; Jorizzo, Joseph L. (2007). Dermatology: 2-Volume Set. St. Louis: Mosby. ISBN 1-4160-2999-0.
{{cite book}}: CS1 maint: multiple names: authors list (link) - ^ MacSweeney STR, Powell JT, Greenhalgh RM (1994). "Pathogenesis of abdominal aortic aneurysm". The British Journal of Surgery. 81 (7): 935–41. doi:10.1002/bjs.1800810704.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Biasetti J, Hussain F, Gasser TC (2011). "Blood flow and coherent vortices in the normal and aneurysmatic aortas: a fluid dynamical approach to intra-luminal thrombus formation". Journal of the Royal Society Interface. 8 (63): 1449. doi:10.1098/rsif.2011.0041.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ a b Fillinger MF, Marra SP, Raghavan ML, Kennedy FE (April 2003). "Prediction of rupture risk in abdominal aortic aneurysm during observation: wall stress versus diameter". Journal of Vascular Surgery. 37 (4): 724–32. doi:10.1067/mva.2003.213. PMID 12663969.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Gasser TC, Auer M, Labruto F, Swedenborg J, Roy J (2010). "Biomechanical rupture risk assessment of abdominal aortic aneurysms: model complexity versus predictability of finite element simulations". Eur J Vasc Endovasc Surg. 40 (2): 176–185. doi:10.1016/j.ejvs.2010.04.003. PMID 20447844.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ http://www.vascops.com/en/vascops-A4clinics.html
- ^ a b U.S. Preventive Services Task Force (2005). "Screening for abdominal aortic aneurysm: recommendation statement". Annals of Internal Medicine. 142 (3): 198–202. PMID 15684208.
- ^ Fleming C, Whitlock EP, Beil TL, Lederle FA (2005). "Screening for abdominal aortic aneurysm: a best-evidence systematic review for the U.S. Preventive Services Task Force". Annals of Internal Medicine. 142 (3): 203–11. PMID 15684209.
{{cite journal}}: CS1 maint: multiple names: authors list (link)ACP Journal Club - ^ Cinà CS, Devereaux PJ (2005). "Review: population-based screening for abdominal aortic aneurysm reduces cause-specific mortality in older men". ACP J. Club. 143 (1): 11. PMID 15989299.
- ^ a b Bown MJ, Sweeting MJ, Brown LC, Powell JT, Thompson SG (February 2013). "Surveillance intervals for small abdominal aortic aneurysms: a meta-analysis". JAMA. 309 (8): 806–13. doi:10.1001/jama.2013.950. PMID 23443444.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ a b c Ballard DJ, Filardo G, Fowkes G, Powell JT (2008). Ballard, David J (ed.). "Surgery for small asymptomatic abdominal aortic aneurysms". Cochrane Database of Systematic Reviews (4): CD001835. doi:10.1002/14651858.CD001835.pub2. PMID 18843626.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Powell JT, Brown LC, Forbes JF; et al. (Jun 2007). "Final 12-year follow-up of surgery versus surveillance in the UK Small Aneurysm Trial". Br J Surg. 94 (6): 702–8. doi:10.1002/bjs.5778. PMID 17514693.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ Lederle FA, Wilson SE, Johnson GR; et al. (May 2002). "Immediate repair compared with surveillance of small abdominal aortic aneurysms". N Engl J Med. 346 (19): 1437–44. doi:10.1056/NEJMoa012573. PMID 12000813.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ Hackam DG, Thiruchelvam D, Redelmeier DA (Aug 2006). "Angiotensin-converting enzyme inhibitors and aortic rupture: a population-based case-control study". Lancet. 368 (9536): 659–65. doi:10.1016/S0140-6736(06)69250-7. PMID 16920471.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Powell JT, Brown LC, Greenhalgh RM, Thompson SG (Jan 2008). "The rupture rate of large abdominal aortic aneurysms: is this modified by anatomical suitability for endovascular repair?". Ann Surg. 247 (1): 173–9. doi:10.1097/SLA.0b013e3181557d2a. PMID 18156938.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Rutherford RB (Jun 2006). "Randomized EVAR trials and advent of level i evidence: a paradigm shift in management of large abdominal aortic aneurysms?". Semin Vasc Surg. 19 (2): 69–74. doi:10.1053/j.semvascsurg.2006.03.001. PMID 16782510.
- ^ Lederle FA, Kane RL, MacDonald R, Wilt TJ (2007). "Systematic review: repair of unruptured abdominal aortic aneurysm". Annals of Internal Medicine. 146 (10): 735–41. PMID 17502634.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Evar Trial Participants (2005). "Endovascular aneurysm repair versus open repair in patients with abdominal aortic aneurysm (EVAR trial 1): randomised controlled trial". Lancet. 365 (9478): 2179–86. doi:10.1016/S0140-6736(05)66627-5. PMID 15978925.
- ^ Blankensteijn JD, de Jong SE, Prinssen M; et al. (Jun 2005). "Two-year outcomes after conventional or endovascular repair of abdominal aortic aneurysms". N Engl J Med. 352 (23): 2398–405. doi:10.1056/NEJMoa051255. PMID 15944424.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ Evar Trial Participants (2005). "Endovascular aneurysm repair and outcome in patients unfit for open repair of abdominal aortic aneurysm (EVAR trial 2): randomised controlled trial". Lancet. 365 (9478): 2187–92. doi:10.1016/S0140-6736(05)66628-7. PMID 15978926.
- ^ Amato ACA, Kahlberg AK, Bertoglio LB, Melissano GM, Chiesa RC (2008). "Endovascular treatment of a triple paraanastomotic aneurysm after aortobiiliac reconstruction". J Vasc Bras. 7 (3): 1–3. doi:10.1590/S1677-54492008000300016.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Endovascular versus open repair of abdominal aortic aneurysm. United Kingdom EVAR Trial Investigators, Greenhalgh RM, Brown LC, Powell JT, Thompson SG, Epstein D, Sculpher MJ. N Engl J Med. 2010 May 20;362(20):1863-71.
- ^ Long-term outcome of open or endovascular repair of abdominal aortic aneurysm. De Bruin JL et al. N Engl J Med 2010;362:1881-9
- ^ A randomized controlled trial of endovascular aneurysm repair versus open surgery for abdominal aortic aneurysms in low- to moderate-risk patients. Becquemin JP et al. J Vasc Surg 2011 May;53(5):1167-1173
- ^ Influence of infrarenal neck length on outcome of endovascular abdominal aortic aneurysm repair. Leurs LJ et al. J Endovasc Ther 2006;13(5):640-8.
- ^ The correlation of aortic neck length to early and late outcomes in endovascular aneurysm repair patients. Aburahma AF et al. J Vasc Surg 2009;50(4):738-48.
- ^ Aortic neck angulation predicts adverse outcome with endovascular abdominal aortic aneurysm repair. Sternbergh WC et al. J Vasc Surg 2002;35(3):482-6.
- ^ Future technologies to address the failed endoprosthesis. Deaton DH. Semin Vasc Surg. 2009 Jun;22(2):111-8.
- ^ Comparison of outcomes with open, fenestrated, and chimney graft repair of juxtarenal aneurysms: are we ready for a paradigm shift? Katsargyris A, Oikonomou K, Klonaris C, Töpel I, Verhoeven EL. J Endovasc Ther. 2013 Apr;20(2):159-69. doi: 10.1583/1545-1550-20.2.159. Review
- ^ Technical aspects, current indications, and results of chimney grafts for juxtarenal aortic aneurysms. Coscas R, Kobeiter H, Desgranges P, Becquemin JP. J Vasc Surg. 2011 Jun;53(6):1520-7.
- ^ Fenestrated endovascular aneurysm repair. Cross J, Gurusamy K, Gadhvi V, Simring D, Harris P, Ivancev K, Richards T. Br J Surg. 2012 Feb;99(2):152-9
- ^ Helical Endostaples Enhance Endograft Fixation in an Experimental Model Using Human Cadaveric Aortas Melas et al J Vasc Surg. 2012;55 (6):1726-1733.
- ^ Improving proximal fixation and seal with the HeliFx Aortic EndoAnchor. Deaton DH. Semin Vasc Surg. 2012 Dec;25(4):187-92
- ^ Rationale of EndoAnchors in abdominal aortic aneurysms with short or angulated necks. De Vries JP et al. J Cardiovasc Surg (Torino). 2014 Feb;55(1):103-7.
- ^ Primary EndoAnchoring in the Endovascular Repair of Abdominal Aortic Aneurysms With an Unfavorable Neck Perdikides et al J Endovasc Ther. 2012; 19.
- ^ Successful Treatment of a Proximal Type I Endoleak with HeliFX EndoAnchors. Hogendoorn W et al. Ann Vasc Surg 2013.
- ^ EndoAnchor Placement in Thoracic and Thoracoabdominal Stent-Grafts to Repair Complications of Nonalignment. Kasprzak P et al. J Endovasc Therapy 2013;20:471-480.
- ^ Use of endostaples to secure migrated endografts and proximal cuffs after failed endovascular abdominal aortic aneurysm repair. de Vries et al J Vasc Surg. 2011;54:1792-1794.
- ^ Bernstein EF, Chan EL (September 1984). "Abdominal aortic aneurysm in high-risk patients. Outcome of selective management based on size and expansion rate". Ann. Surg. 200 (3): 255–63. doi:10.1097/00000658-198409000-00003. PMC 1250467. PMID 6465980.
- ^ Brewster DC, Cronenwett JL, Hallett JW, Johnston KW, Krupski WC, Matsumura JS (May 2003). "Guidelines for the treatment of abdominal aortic aneurysms. Report of a subcommittee of the Joint Council of the American Association for Vascular Surgery and Society for Vascular Surgery". J. Vasc. Surg. 37 (5): 1106–17. doi:10.1067/mva.2003.363. PMID 12756363.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Darling RC, Messina CR, Brewster DC, Ottinger LW (September 1977). "Autopsy study of unoperated abdominal aortic aneurysms. The case for early resection". Circulation. 56 (3 Suppl): II161–4. PMID 884821.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ a b Nicholls SC, Gardner JB, Meissner MH, Johansen HK (November 1998). "Rupture in small abdominal aortic aneurysms". Journal of Vascular Surgery. 28 (5): 884–8. doi:10.1016/S0741-5214(98)70065-5. PMID 9808857.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ a b Vorp DA (2007). "BIOMECHANICS OF ABDOMINAL AORTIC ANEURYSM". Journal of Biomechanics. 40 (9): 1887–902. doi:10.1016/j.jbiomech.2006.09.003. PMC 2692528. PMID 17254589.
- ^ Vorp DA, Raghavan ML, Webster MW (April 1998). "Mechanical wall stress in abdominal aortic aneurysm: influence of diameter and asymmetry". Journal of Vascular Surgery. 27 (4): 632–9. doi:10.1016/S0741-5214(98)70227-7. PMID 9576075.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Sacks MS, Vorp DA, Raghavan ML, Federle MP, Webster MW (1999). "In vivo three-dimensional surface geometry of abdominal aortic aneurysms". Annals of Biomedical Engineering. 27 (4): 469–79. doi:10.1114/1.202. PMID 10468231.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ a b Doyle BJ, Callanan A, Burke PE; et al. (February 2009). "Vessel Asymmetry as an Additional Diagnostic Tool in the Assessment of Abdominal Aortic Aneurysms". Journal of Vascular Surgery. 49 (2): 443–54. doi:10.1016/j.jvs.2008.08.064. PMC 2666821. PMID 19028061.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ Geest, Vande J.P.; Wang, D.H.J.; Wisniewski, S.R.; Makaroun, M.S.; Vorp, D.A. (2006). "Towards A Noninvasive Method for Determination of Patient-Specific Wall Strength Distribution in Abdominal Aortic Aneurysms". Annals of Biomedical Engineering. 34 (7): 1098–1106. doi:10.1007/s10439-006-9132-6. PMID 16786395.
- ^ Raghavan ML, Kratzberg J, Castro de Tolosa EM, Hanaoka MM, Walker P, da Silva ES (2006). "Regional distribution of wall thickness and failure properties of human abdominal aortic aneurysm". Journal of Biomechanics. 39 (16): 3010–6. doi:10.1016/j.jbiomech.2005.10.021. PMID 16337949.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Raghavan ML, Webster MW, Vorp DA (1996). "Ex vivo biomechanical behavior of abdominal aortic aneurysm: assessment using a new mathematical model". Annals of Biomedical Engineering. 24 (5): 573–82. doi:10.1007/BF02684226. PMID 8886238.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Thubrikar MJ, Labrosse M, Robicsek F, Al-Soudi J, Fowler B (2001). "Mechanical properties of abdominal aortic aneurysm wall". Journal of Medical Engineering & Technology. 25 (4): 133–42. doi:10.1080/03091900110057806. PMID 11601439.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Fillinger MF, Raghavan ML, Marra SP, Cronenwett JL, Kennedy FE (September 2002). "In vivo analysis of mechanical wall stress and abdominal aortic aneurysm rupture risk". Journal of Vascular Surgery. 36 (3): 589–97. doi:10.1067/mva.2002.125478. PMID 12218986.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Venkatasubramaniam AK, Fagan MJ, Mehta T; et al. (August 2004). "A comparative study of aortic wall stress using finite element analysis for ruptured and non-ruptured abdominal aortic aneurysms". European Journal of Vascular and Endovascular Surgery. 28 (2): 168–76. doi:10.1016/j.ejvs.2004.03.029. PMID 15234698.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ Hirose Y, Takamiya M (February 1998). "Growth curve of ruptured aortic aneurysm". The Journal of Cardiovascular Surgery. 39 (1): 9–13. PMID 9537528.
- ^ Wang DH, Makaroun MS, Webster MW, Vorp DA (September 2002). "Effect of intraluminal thrombus on wall stress in patient-specific models of abdominal aortic aneurysm". Journal of Vascular Surgery. 36 (3): 598–604. doi:10.1067/mva.2002.126087. PMID 12218961.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Vorp DA, Vande Geest JP (August 2005). "Biomechanical determinants of abdominal aortic aneurysm rupture". Arteriosclerosis, Thrombosis, and Vascular Biology. 25 (8): 1558–66. doi:10.1161/01.ATV.0000174129.77391.55. PMID 16055757.
- ^ Geest, Vande J.P.; Martino, Di E.S.; Bohra, A.; Makaroun, M.S.; Vorp, D.A. (2006). "A biomechanics-based rupture potential index for abdominal aortic aneurysm risk assessment". Annals of the New York Academy of Sciences. 1085: 11–21. doi:10.1196/annals.1383.046. PMID 17182918.
- ^ Doyle, B.J.; Callanan, A.; Walsh, M.T.; Grace, P.A.; McGloughlin, T.M. (2009). "A finite element analysis rupture index (FEARI) as an additional tool for abdominal aortic aneurysm rupture prediction". Vascular Disease Prevention. 6: 114–121. doi:10.2174/1567270000906010114.
- ^ Kleinstreuer C, Li Z (2006). "Analysis and computer program for rupture-risk prediction of abdominal aortic aneurysms". Biomedical Engineering Online. 5: 19. doi:10.1186/1475-925X-5-19. PMC 1421417. PMID 16529648.
{{cite journal}}: CS1 maint: unflagged free DOI (link) - ^ Stenbaek J, Kalin B, Swedenborg J (November 2000). "Growth of thrombus may be a better predictor of rupture than diameter in patients with abdominal aortic aneurysms". European Journal of Vascular and Endovascular Surgery. 20 (5): 466–9. doi:10.1053/ejvs.2000.1217. PMID 11112467.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Giannoglou G, Giannakoulas G, Soulis J; et al. (2006). "Predicting the risk of rupture of abdominal aortic aneurysms by utilizing various geometrical parameters: revisiting the diameter criterion". Angiology. 57 (4): 487–94. doi:10.1177/0003319706290741. PMID 17022385.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ Watton PN, Hill NA, Heil M (November 2004). "A mathematical model for the growth of the abdominal aortic aneurysm". Biomechanics and Modeling in Mechanobiology. 3 (2): 98–113. doi:10.1007/s10237-004-0052-9. PMID 15452732.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Volokh KY, Vorp DA (2008). "A model of growth and rupture of abdominal aortic aneurysm". Journal of Biomechanics. 41 (5): 1015–21. doi:10.1016/j.jbiomech.2007.12.014. PMID 18255074.
- ^ Greenhalgh RM, Brown LC, Kwong GP, Powell JT, Thompson SG (2004). "Comparison of endovascular aneurysm repair with open repair in patients with abdominal aortic aneurysm (EVAR trial 1), 30-day operative mortality results: randomised controlled trial". Lancet. 364 (9437): 843–8. doi:10.1016/S0140-6736(04)16979-1. PMID 15351191.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Salem MK, Rayt HS, Hussey G; et al. (December 2009). "Should Asian men be included in abdominal aortic aneurysm screening programmes?". Eur J Vasc Endovasc Surg. 38 (6): 748–9. doi:10.1016/j.ejvs.2009.07.012. PMID 19666232.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ Creager, MA, Halperin, JL, Whittemore, AD (1996). "Aneurysmal disease of the aorta and its branches". In Loscalzo, J, Creager, MA, Dzau, VJ (ed.). Vascular Medicine. New York: Little, Brown. p. 901.
{{cite book}}: CS1 maint: multiple names: authors list (link) - ^ Wilmink TB, Quick CR, Day NE (Dec 1999). "The association between cigarette smoking and abdominal aortic aneurysms". J Vasc Surg. 30 (6): 1099–105. doi:10.1016/S0741-5214(99)70049-2. PMID 10587395.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Baird PA, Sadovnick AD, Yee IM, Cole CW, Cole L (Sep 1995). "Sibling risks of abdominal aortic aneurysm". Lancet. 346 (8975): 601–4. doi:10.1016/S0140-6736(95)91436-6. PMID 7651004.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Livesay JJ, Messner GN, Vaughn WK (2005). "Milestones in Treatment of Aortic Aneurysm: Denton A. Cooley, MD, and the Texas Heart Institute". Tex Heart Inst J. 32 (2): 130–4. PMC 1163455. PMID 16107099.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Famous Patients, Famous Operations, 2002 — Part 3: The Case of the Scientist with a Pulsating Mass from Medscape Surgery
- ^ Yusuf SW, Whitaker SC, Chuter TA, Wenham PW, Hopkinson BR (December 1994). "Emergency endovascular repair of leaking aortic aneurysm". Lancet. 344 (8937): 1645. doi:10.1016/S0140-6736(94)90443-X. PMID 7984027.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ a b "Bob Dole has surgery to treat aneurysm". USA Today via Associated Press. 2001-06-27. Retrieved 2009-09-22.
{{cite news}}: Italic or bold markup not allowed in:|publisher=(help) - ^ Raghavan, M.L.; Kratzberg, J.; Tolosa, de E.M.C.; Hanaoka, M.M.; Walter, P.; Silva, da E.S. (2006). "Regional distribution of wall thickness and failure properties of human abdominal aortic aneurysm". J. Biomech. 39 (16): 3010–3016. doi:10.1016/j.jbiomech.2005.10.021. PMID 16337949.
- ^ Vorp, D.A.; Lee, P.C.; Wang, D.H.J.; Makaroun, M.S.; Nemoto, E.M.; Ogawa, S.; Webster, M.W. (2001). "Association of intraluminal thrombus in abdominal aortic aneurysm with local hypoxia and wall weakening". Journal of Vascular Surgery. 34 (2): 291–299. doi:10.1067/mva.2001.114813. PMID 11496282.
- ^ Speelman, L.; Bohra, A.; Bosboom, E.M.H.; Schurink, G.W.H.; Vosse, van de F.N.; Makaroun, M.S.; Vorp, D.A. (2007). "Effects of wall calcifications in patient-specific wall stress analyses of abdominal aortic aneurysms". Journal of Biomechanical Engineering. 129 (1): 105–109. doi:10.1115/1.2401189. PMID 17227104.
- ^ Doyle, B.J.; Morris, L.G.; Callanan, A.; Kelly, P.; Vorp, D.A.; McGloughlin, T.M. (2008). "3D reconstruction and manufacture of real abdominal aortic aneurysms: From CT scan to silicone model". Journal of Biomechanical Engineering. 130 (3): 034501. doi:10.1115/1.2907765. PMID 18532870.
- ^ Doyle, B.J.; Corbett, T.J.; Cloonan, A.J.; O'Donnell, M.R.; Walsh, M.T.; Vorp, D.A.; McGloughlin, T.M. (2009). "Experimental mOdelling of Aortic Aneurysms: Novel applications of Silicone Rubbers". Medical Engineering & Physics. 31 (8): 1002–1012. doi:10.1016/j.medengphy.2009.06.002. PMC 2757445. PMID 19595622.
- ^ Morris, L.; O'Donnell, P.; Delassus, P.; McGloughlin, T.M. (2004). "Experimental assessment of stress patterns in abdominal aortic aneurysms using the photoelastic method". Strain. 40 (4): 165–172. doi:10.1111/j.1475-1305.2004.tb01425.x.
- ^ Doyle, B.J.; Corbett, T.J.; Callanan, A.; Walsh, M.T.; Vorp, D.A.; McGloughlin, T.M. (2009). "An Experimental and Numerical Comparison of the Rupture Locations of an Abdominal Aortic Aneurysm". Journal of Endovascular Therapy. 16 (3): 322–335. doi:10.1583/09-2697.1. PMC 2795364. PMID 19642790.
- ^ Albertini JN, Perdikides T, Soong CV, Hinchliffe RJ, Trojanowska M, Yusuf SW (Jun 2006). "Endovascular repair of abdominal aortic aneurysms in patients with severe angulation of the proximal neck using a flexible stent-graft: European Multicenter Experience". J Cardiovasc Surg (Torino). 47 (3): 245–50. PMID 16760860.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ "Study establishes major new treatment target in diseased arteries". U.S. News & World Report. May 10, 2009.
- ^ Attention: This template ({{cite doi}}) is deprecated. To cite the publication identified by doi:10.2353/ajpath.2010.090700, please use {{cite journal}} (if it was published in a bona fide academic journal, otherwise {{cite report}} with
|doi=10.2353/ajpath.2010.090700instead. - ^ "Discovery points way for new treatment for aneurysms". University of British Columbia. January 27, 2010.